Personal Development Plans
Because "I'll learn everything eventually" isn't a plan — it's a hope. And hope, bless it, doesn't get signed off at ARCP.
The PDP (Personal Development Plan) is one of those ePortfolio boxes that trainees tend to leave until the night before their ESR. This page changes that. Whether you've never written one, or you've been writing them vaguely for years, here is everything you need to write a PDP that actually means something — for your training, your ARCP, and beyond.
📅 Last updated: April 2026
Jump to a section
📥 Downloads
Handouts, templates, and examples — ready to use in clinic, tutorials, or that ESR you've been putting off.
path: PDPs
🌐 Web Resources
A hand-picked mix of official guidance and real-world GP training resources.
⚡ If You Only Read One Thing…
- A PDP = your plan for tackling bigger, chunkier learning needs — not a learning log and not a to-do list
- RCGP minimum: 2 PDPs per training year, with progress demonstrated in at least one; good practice is 3+ per clinical placement
- Every PDP must be SMART — vague goals fail ARCP panels; "Pass AKT" and "write more log entries" are explicitly unacceptable
- All learning is Knowledge, Skills, or Attitudes (KSA) — know which one you're working on and state it
- Use the Gold Standard Loop: Case → Reflection → PDP → Learning → Evidence → Application → Review → Repeat
- Aim for breadth across all five RCGP capability areas — not just Area B (clinical knowledge)
- A poor PDP has delayed trainee CCT applications at ARCP — this genuinely matters
- From August 2025: PDPs should reflect the updated RCGP curriculum — virtual consulting, planetary health, health equity, co-produced care
- The PDP you finish training with becomes the foundation of your lifelong appraisal and revalidation cycle
🎯 Why the PDP Actually Matters
It's not just admin. Here's why it genuinely counts.
Many trainees treat the PDP as an afterthought — something to fill in quickly before the ESR so it doesn't look empty. That's understandable. It's also a mistake.
ARCP Impact
ARCP panels look at your PDP as evidence of self-directed learning. An empty or static PDP is a red flag. Some trainees have had their CCT delayed because of a consistently poor PDP. Outcome 2 (additional requirements) and Outcome 3 (extra training time) can both be influenced by PDP quality.
Lifelong Learning
The PDP you finish training with becomes the backbone of your lifelong appraisal and revalidation cycle. Under GMC requirements, all licensed GPs must demonstrate CPD and reflective practice. The habits you build now are the foundation of safe ongoing practice.
Focused Development
GP training is vast. The PDP is what stops you drifting and helps you concentrate energy where it genuinely matters — especially in areas where you feel less confident.
Revalidation Ready
Active PDPs are mandatory for appraisal. Completed appraisals are mandatory for revalidation. Start building the habit now, while you have a supervisor around to help you.
The trainees who find PDPs easy treat them as genuinely useful — not as a hoop to jump through. When you identify a real gap and map out a real plan, writing the PDP becomes natural. The trainees who struggle are the ones writing it at 11pm the night before their ESR.
📖 What Is a PDP?
And — equally important — what it is NOT.
The PDP (Personal Development Plan) is an educational tool within your ePortfolio that helps you document your bigger, chunkier learning needs — the ones that require planning, time, and multiple steps to address.
❌ PDP is NOT…
… a learning log (that's for everyday clinical encounters)
… "Pass AKT" or "Write more log entries" — explicitly unacceptable per RCGP
… something you write once and forget
✅ PDP IS…
… a structured plan for your bigger learning goals
… needs-driven, grounded in real clinical experience
… SMART and specific, with evidence of achievement
… a living document that evolves during the post
… the foundation of your post-CCT appraisal
Learning log: "Today I saw a patient with gout and I didn't know the first-line management. I read the NICE CKS afterwards." — done in an evening.
PDP entry: "I've realised from multiple learning logs that I lack confidence in women's health. I'm going to sit in with the practice's women's health lead, attend a menopause course, and complete three relevant CBDs." — needs weeks and planning.
Where do PDP entries come from?
- Learning logs that identify recurring gaps — use the "Send to PDP" button on FourteenFish
- Patient encounters that exposed a knowledge or skills deficit
- PUNs (Patient Unmet Needs) and DENs (Doctor's Educational Needs)
- Feedback from CBD/COT/Mini-CEX assessments and MSF
- RCGP GP SelfTest — curriculum-wide learning needs assessment
- Placement planning meeting — self-assessment against specialty handbook tool
- ESR capability ratings — "Needs Further Development" must generate a PDP entry
How many PDPs do I need?
RCGP minimum: 2 per training year, with progress demonstrated in at least one. Good practice: 3 per clinical placement. Quality beats quantity every time.
How PDPs work on FourteenFish — the sequential order trap
The three stages must be completed in order. Skipping Stage 1 means your previous entries disappear from Stage 2, and entries not agreed at Stage 3 won't appear at the next ESR:
- Review progress against previously agreed PDP goals
At ESR preparation — carry forward or close existing entries before moving on.
- Suggest new PDP entries
In the ESR preparation area — propose new goals for the next review period.
- Agree the PDP with your Educational Supervisor
At the ESR — co-construct the agreed goals for the coming review period.
🧠 What Type of Learning Is It?
All learning fits into one of three categories. Know which one you're targeting.
Every PDP entry addresses a learning need that falls into at least one of three categories: Knowledge, Skills, or Attitudes (KSA). Being explicit about which category your PDP targets helps you write sharper goals.
Knowledge
Learning new facts, understanding guidelines, reading around a topic.
e.g. "Improve understanding of NICE contraception guidance — LARC options, COC contraindications, and emergency contraception."
Skills
Practical abilities, consultation skills, communication techniques, clinical examination.
e.g. "Develop motivational interviewing techniques for lifestyle change consultations — practise in clinic, evidence via COT."
Attitudes
Shifts in perspective, values, professional approach, cultural awareness.
e.g. "After a tutorial on health inequalities, explore how unconscious bias affects my consulting — evidence via reflection."
State explicitly whether your goal is K, S, or A. It demonstrates self-awareness and makes your learning plan far more specific. A goal that covers all three can be powerful — just be clear about what you're trying to achieve from each angle.
✨ The SMARTIES Framework
Your blueprint for writing PDP entries that pass muster.
Every PDP entry should pass each of these eight checks. If your goal fails any of them, it needs rewriting before your supervisor or ARCP panel sees it.
Specific
Relates to a specific task or area — not a vague general statement.
✗ "Improve consultation skills" → ✓ "Learn and apply motivational interviewing in lifestyle change consultations"
Measurable
You can assess whether it's been achieved — there's a clear endpoint.
✗ "Show improvement" → ✓ "Complete a COT and write up 3 reflections on using MI techniques"
Achievable
Realistic within your current post and circumstances.
✗ "Learn everything about women's health" → ✓ "Improve knowledge of contraception, menstruation disorders, and menopause"
Relevant
Relevant to your current role, your patients, and the RCGP curriculum.
✗ "Learn rare neurological conditions" → ✓ "Improve knowledge of MS management in primary care"
Time-bound
A clear deadline. "Soon" is not a date. "By September 2026" is.
✗ "Will attend a course at some point" → ✓ "Registered for Women's Health course, September 2026"
Inspirational
Motivates you to actually do it. Dull goals gather dust.
Choose an area you find genuinely interesting, or where a real patient encounter moved you — the learning sticks better.
Emotional
Connected to a real experience — a patient encounter, a near-miss, a moment that stayed with you.
The best PDPs often start: "I saw a patient with X and I realised I wasn't sure how to manage Y…"
Successful
Completable — and once done, demonstrable with evidence.
State upfront: "I will demonstrate this with a completed CBD, reflective log, and course certificate."
🧩 SMAARTER+ — The Extended Framework
SMAARTER+ adds Evaluated, Reviewed, and + Impact documented — the three elements ARCP panels most often find missing.
| Letter | Stands For | What It Means in Practice |
|---|---|---|
| S | Specific | Name the exact skill, condition, or behaviour — not a general domain |
| M | Measurable | Clear endpoint — evidenced by something tangible |
| A | Achievable | Realistic within your current post and circumstances |
| A | Aligned to curriculum | Linked to an RCGP capability area — explicitly stated where possible |
| R | Relevant | Relevant to your current role, patients, and stage of training |
| T | Time-bound | A specific deadline — a month and year, not "soon" |
| E | Evaluated | You have assessed whether the learning was achieved — not just assumed it was |
| R | Reviewed | You have revisited the goal during the post — updated, progressed, or closed it |
| + | Impact documented | You have recorded what actually changed in your practice as a result |
🛠️ Quick PDP Builder — Five Steps From Gap to Goal
- Identify the gap
What specifically do you not know, cannot do well, or find yourself avoiding? One gap per PDP entry.
- Link it to a case or log entry
Which patient encounter, feedback, or assessment triggered this? Reference it explicitly.
- Add the guideline or framework
For knowledge gaps: name the specific NICE CKS topic or BNF section. For skills: name the model (e.g. Calgary-Cambridge, SPIKES).
- Define the specific action and deadline
What exactly will you do, and by when? Name the course, the clinic, the colleague. Date it specifically.
- Define the outcome and evidence
What will you produce as evidence? What will have changed in your practice?
GAP → CASE → GUIDELINE → ACTION + DATE → OUTCOME + EVIDENCE
✅ Good vs Bad PDP Examples
The difference between a PDP that impresses and one that quietly underwhelms.
📋 General PDP Goals — Weak vs Strong
| WHAT (Goal) | HOW (Actions) | WHEN | OUTCOME (Evidence) | Verdict |
|---|---|---|---|---|
| Keep up to date with new clinical developments | Attend tutorials | Over next 6–12 months | Pass exams | ❌ Fails all SMART criteria |
| Learn about gynaecology as applied to general practice | Attend tutorials and ward rounds during O&G job | Over next 6 months | Be more confident | ❌ Too broad — "confident" unmeasurable |
| Become more proficient in taking sexual health histories (from patient encounter during GU placement) | Practice in joint consultations with GU nurse; targeted reading | During GU attachment (July–Sept 2026) | CBD and Mini-CEX, plus written reflection | ✅ Specific, measurable, time-bound, linked to experience |
| Develop knowledge and skills in motivational interviewing for lifestyle change consultations | Complete MI online course; apply in clinic; reflect on 3 consultations; discuss in tutorial | Course by Aug 2026; reflections by Oct 2026 | Course certificate; 3 annotated log entries; COT demonstrating MI techniques | ✅ Excellent — clear KSA, SMART, evidence mapped out |
🧠 SMART Goals — Applied to GP Training
| Letter | Meaning | GP Training Application | ❌ Vague | ✅ SMART Version |
|---|---|---|---|---|
| S | Specific | Name the exact skill, condition, or behaviour | "Improve knowledge of hypertension" | "Review 10 hypertension patients I've managed and get trainer feedback on appropriateness of management decisions" |
| M | Measurable | Specific portfolio evidence — log entry, CBD, COT | "Study for my AKT" | "Complete 1 hour AKT practice questions daily, cover 3 curriculum topics per week for 3 months via RCGP GP SelfTest" |
| A | Achievable | Resource realistically available in this rotation? | "Improve women's health knowledge" | "Improve knowledge of contraception options — evidenced by a CBD with trainer and a learning log reflection" |
| R | Relevant | Relevant to your needs and future GP practice | "Increase confidence in paediatrics" | "Attend paediatric A&E clinic x4, complete 2 CbDs, write reflection on common presentations in primary care" |
| T | Time-bound | Name a specific target month and year | "Add more log entries" ← explicitly unacceptable | Any goal with a named month/year and named evidence type |
🎯 SCA Consultation Skills — Weak vs Strong
❌ Weak SCA PDP
Goal: "Improve my empathy in consultations."
Action: "Be more empathetic."
Evidence: (blank)
No specific behaviour, no measurable action, no evidence planned.
✅ Strong SCA PDP
Goal: "Develop interpretive empathy — naming and reflecting the patient's emotional experience rather than using generic phrases."
Action: "Practise reflective statements in 5+ consultations per week. Two COTs with trainer."
Evidence: "Two COTs with feedback; five annotated log entries."
By: End October 2026.
Read your PDP back and ask: "How would I know if I'd achieved this?" If you cannot answer that clearly, the goal needs rewriting. For consultation skills goals, add: "What specific behaviour am I trying to change — and how will anyone observe that change?"
✍️ How to Write a PDP Entry
A practical, step-by-step walkthrough.
- Identify the need from a real experience
Start with what triggered the learning need — a patient encounter, a learning log, feedback, an ESR capability rating, or your RCGP GP SelfTest results. Reference it explicitly. The PDP should feel like it grew out of real practice, not thin air.
- Define what you want to learn (Knowledge, Skills, or Attitudes)
State explicitly which of KSA this addresses. Be specific — not "learn about diabetes" but "improve my knowledge of insulin initiation in type 2 diabetes in primary care, and when to refer."
- Plan the specific actions you'll take
Name the steps: a course, supervised practice, reading specific guidelines, sitting in with a colleague, completing a targeted CBD. Concrete actions are far more convincing than vague plans.
- Set a deadline for each action
Give each action a specific date. "By September 2026" is a deadline. "Soon" is not. Better still — book things in now and note the confirmed date.
- State what evidence you'll provide
Plan upfront: certificate, learning log reflections, CBD, COT, Mini-CEX. Make it easy for your supervisor to see that you've done what you planned.
- State how you'll know you've achieved it — and write a follow-up CCR
Keep it simple: "I will be able to manage this independently." Then write a follow-up clinical case review showing you applied the learning. This closes the loop — the step that most distinguishes high-quality portfolios.
- Update it during the post
Set two diary reminders per review period — at 6 weeks and 10 weeks. Update as you complete activities. A dynamic PDP impresses far more than a static one.
When writing a learning log (CCR), if it identifies a significant learning need, use the "Send to PDP" button. This pre-populates the PDP entry with context from your log — saving time and ensuring the need is grounded in a real clinical experience. Do it at the time, not weeks later.
📂 PDP Ideas Database
Grouped by RCGP capability area and by rotation — to help you get started.
Use these examples as starting points, not templates to copy verbatim. Remember: most trainees cluster PDPs around Capability Area B (clinical knowledge) — actively choose from Areas A, D, and E to demonstrate breadth.
By RCGP Capability Area
Area A — Communicating, Consulting & Ethical Practice
- Develop motivational interviewing techniques for lifestyle change consultations — practise in clinic, evidence via COT and learning log reflections
- Improve interpretive empathy — replace generic phrases with statements that name the patient's emotional experience; evidence via COT with trainer feedback
- Improve ability to deliver difficult news using a structured framework (e.g. SPIKES); practise in observed consultations
- Develop skills in shared decision-making — presenting options clearly, eliciting patient preferences; evidence via CBD
- Improve understanding of consent and capacity under the Mental Capacity Act 2005
- Develop virtual and remote consulting competence — practise telephone and video consultation safety-netting; evidence via clinical supervisor feedback
Area B — Clinical Knowledge & Decision-Making
- Improve structured approach to the undifferentiated presentation — using a systematic framework to avoid anchoring too early on one diagnosis
- Improve knowledge of contraception options including LARC — indications, contraindications, fitting referral pathways; evidence via CBD
- Develop systematic approach to managing type 2 diabetes — HbA1c targets (48/53/58 mmol/mol), SGLT-2 inhibitor indications, and when to consider insulin; evidence via CBD
- Improve knowledge of musculoskeletal conditions — shoulder, knee, and lower back pain; examination findings, management, and referral thresholds
- Develop knowledge in primary care dermatology — common rashes, skin cancer recognition, 2WW criteria, and when to refer urgently
- Improve understanding of the menopause — assessment, HRT options, contraindications, and monitoring; evidence via CBD and course certificate
- Improve understanding of palliative care in primary care — symptom management, anticipatory prescribing, coordination with specialist teams
Area C — Managing Complex & Long-Term Care
- Develop confidence in managing patients with multiple long-term conditions — prioritisation, structured reviews, avoiding polypharmacy; evidence via CBD
- Improve understanding of safeguarding — children and adults — specifically recognition, documentation, and referral pathways
- Develop skills in team-based care — understanding roles of other professionals in the PCN
Area D — Leadership, Teaching & Organisational Learning
- Develop teaching skills — learn how to give structured feedback, design a learning objective, and facilitate a tutorial
- Initiate a QIA/QIP in collaboration with the practice team — from identifying the gap through data collection to implementing change and re-audit
- Develop prescribing safety competence — complete prescribing trainee assessment and reflect on prescribing decisions in three CCRs
- Develop understanding of NHS primary care structures — how practices, PCNs, and ICBs interact; evidence via reflective log
Area E — Holistic Care, Health Promotion & Sustainability
- Develop awareness of planetary health in prescribing — specifically inhaler selection with carbon footprint considerations; evidence via CBD and guideline review
- Develop skills in co-produced care plans for patients with long-term conditions — involving patients meaningfully in goal-setting
- Develop understanding of health inequalities in my patient population — how deprivation, ethnicity, and access barriers affect health outcomes
- Explore my own wellbeing and resilience — identify sustainable working habits; evidence via reflection and discussion with trainer
By Hospital Rotation — GP-Framed PDP Ideas (Alphabetical)
During hospital rotations, always reframe the learning need in GP terms: not "what will I learn in this specialty?" but "how will this help me as a GP?"
| Rotation | GP-Relevant PDP Example | Evidence Type |
|---|---|---|
| Accident & Emergency | "Improve management of acutely unwell patients presenting to primary care — complete ABCDE structured assessments x5 and evidence via Mini-CEX with Clinical Supervisor; reflect on presentations that could have been managed in primary care without ED attendance" | Mini-CEX x5, CCR |
| Dermatology | "Improve recognition and management of common skin conditions in primary care — specifically eczema step-up therapy, appropriate use of topical corticosteroids by potency, recognition of suspicious lesions, and 2WW referral criteria; evidence via CCR and supervised skin clinic sessions" | CCR, supervised clinic log |
| Elderly Medicine | "Improve ability to initiate advance care planning discussions and manage frailty in primary care — attend ACP clinic x3 and complete a CBD with trainer; reflect on medication review in the older patient and polypharmacy management" | CBD, CCR, ACP clinic log |
| ENT (Ear, Nose & Throat) | "Develop ability to manage common ENT presentations in primary care — specifically acute otitis media, epistaxis management and advice, appropriate antibiotic thresholds for tonsillitis, and 2WW criteria for suspected head and neck cancer; evidence via CCR and trainer feedback" | CCR, CBD |
| Gastroenterology | "Improve knowledge of common gastrointestinal conditions in primary care — specifically IBS diagnosis and management (Rome IV criteria), GORD step-up therapy, 2WW lower GI cancer criteria, and appropriate use of FIT testing; evidence via CBD and CCR reflecting application in GP setting" | CBD, CCR |
| General Medicine | "Improve structured approach to managing patients with multiple long-term conditions encountered in primary care — specifically polypharmacy review, appropriate monitoring of chronic disease, and recognising when hospital-level input is needed; evidence via CBD and CCR reflecting cases applicable to future GP practice" | CBD, CCR |
| Neurology | "Develop confidence in recognising and initially managing common neurological presentations in primary care — specifically migraine versus red flag headache, TIA pathway (FAST+ criteria, ABCD2 score, urgent referral), and first seizure management including driving advice; evidence via CBD and CCR" | CBD, CCR |
| Obstetrics & Gynaecology | "Achieve competency in counselling patients regarding emergency contraception options including IUCD — evidence via CEPS and CbD; improve knowledge of obstetric red flags in early pregnancy relevant to primary care" | CEPS, CBD, CCR |
| Ophthalmology | "Improve ability to recognise and appropriately triage acute eye presentations in primary care — specifically acute angle closure glaucoma, central retinal artery occlusion, and giant cell arteritis; understand when same-day referral vs routine referral is appropriate; evidence via CCR and direct observation with ophthalmology supervisor" | CCR, supervisor observation log |
| Paediatrics | "Improve recognition of serious illness in children and ability to manage the acutely unwell child in primary care — including NICE traffic light system for febrile children, safeguarding recognition, and appropriate safety-netting for parents; evidence via Mini-CEX and CCR" | Mini-CEX, CCR x2 |
| Palliative Care | "Develop skills in managing end-of-life care in primary care — specifically symptom control in the last days of life, anticipatory prescribing (including appropriate drugs for a syringe driver), recognising the dying patient, and initiating goals of care conversations; evidence via CBD and CCR with palliative care supervisor" | CBD, CCR |
| Psychiatry | "Develop ability to assess suicide risk using a structured approach and manage mental health crises in primary care — specifically the risk assessment framework, appropriate use of the Mental Health Act, and crisis referral pathways; evidence via CbD and CCR" | CBD, CCR, reflection |
| Renal Medicine | "Improve understanding of CKD management in primary care — specifically monitoring intervals, medication adjustments required (ACE inhibitors, NSAIDs, metformin, potassium-sparing diuretics), NICE referral criteria (ACR >70, rapid decline), and interpretation of renal blood results; evidence via CBD reflecting a CKD patient managed in GP" | CBD, CCR |
| Rheumatology | "Improve recognition and initial management of inflammatory arthritis in primary care — specifically early rheumatoid arthritis (morning stiffness, small joint involvement, anti-CCP), monitoring toxicity in patients on DMARD therapy (methotrexate, hydroxychloroquine), and urgent referral criteria; evidence via CBD and CCR" | CBD, CCR |
| Urology | "Improve management of common urological presentations in primary care — specifically recurrent UTI (investigation and prevention), macroscopic haematuria referral pathway (2WW criteria), and benign prostatic hyperplasia management including alpha-blockers and when to refer; evidence via CBD and CCR" | CBD, CCR |
| GP Post (ST1/ST2) | "Improve structured approach to QIA/audit — initiate a QIP in collaboration with practice team; document learning in a QIA reflective log" | QIA log, team feedback |
| GP Post (ST3) | "Develop prescribing safety competence — complete prescribing trainee assessment and reflect on prescribing decisions in x3 CCRs; discuss with Educational Supervisor" | Prescribing assessment, CCR x3 |
For every PDP during a hospital rotation, ask: "How does this help me as a future GP?" Learning LSCS technique is not GP-relevant. Counselling patients about elective LSCS, risks, and recovery is. Planning to perform lumbar punctures is not GP-relevant. Recognising meningism and knowing when to admit urgently is.
A comprehensive database of PDP action points mapped to each RCGP Professional Capability is available in the Downloads section above — and also on the Bradford VTS Action Points page.
📋 PDP Requirements & Curriculum Framework
What the RCGP requires, how to align your PDPs to capabilities, and staying current with the 2025 curriculum update.
📋 PDP Mandatory Minimums
| Requirement | Detail |
|---|---|
| Minimum PDPs per training year | 2, with progress demonstrated in at least one |
| Good practice (per clinical placement) | 3 per clinical placement — aim for this, not the minimum |
| Who agrees the PDP? | The trainee and their Educational Supervisor, jointly at the ESR |
| What must each entry contain? | Learning need + action plan + target date + how success will be demonstrated |
| When is PDP reviewed? | At each ESR (6-monthly); progress updated throughout the review period |
| Not acceptable as PDP entries | "Pass the AKT/SCA", "Add more log entries" — national requirements, not personal learning needs |
The three stages must be completed in order: (1) Review progress → (2) Suggest new entries → (3) Agree with ES. If you skip Stage 1, previous entries disappear from Stage 2. If you skip Stage 3, entries won't appear in Step 1 at the next review. This catches many trainees off guard.
✍️ Writing Up PDP Items Related to AKT
When AKT practice questions or clinical gaps reveal a knowledge deficit, convert it into a specific, evidenced PDP entry. The examples below show the difference between a vague reaction to a knowledge gap and a well-constructed PDP goal.
❌ Vague Reaction to a Gap
"I need to revise diabetes."
Not a PDP entry. This is a vague intention with no action, no timeline, and no way of knowing when it's been achieved.
✅ Well-Constructed PDP Goal
"Review NICE type 2 diabetes guidelines — HbA1c targets (48/53/58 mmol/mol), SGLT-2 inhibitor indications, and when to consider insulin initiation in primary care; evidence via CBD and CCR."
❌ Vague Topic Area
"Improve dermatology knowledge."
The AKT and real clinical practice tests a specific rash, a specific referral threshold, or a specific treatment — not a topic area in general.
✅ Specific, Targeted Goal
"Review NICE CKS eczema management — step-up therapy, topical steroid potency by area, and when to refer for patch testing or specialist review; evidence via CCR and supervisor discussion."
🎯 Gold Standard PDP Goals — Examples
| Weak PDP Goal | Strong, Specific PDP Goal |
|---|---|
| ❌ "Revise asthma" | ✅ "Review NICE asthma stepwise management — MART therapy indications, SABA overuse risks, and when to step up from ICS alone; evidence via CBD" |
| ❌ "Read about hypertension" | ✅ "Review NICE hypertension BP targets (<140/90 under 80; <150/90 over 80), ABPM thresholds, and first-line treatment by age and ethnicity; evidence via review of 10 patients I have managed" |
| ❌ "Improve cancer referral knowledge" | ✅ "Review 2WW criteria for colorectal cancer — symptom-age combinations, FIT ≥10 threshold, and when urgent direct access applies; evidence via CBD and CCR" |
| ❌ "Improve women's health knowledge" | ✅ "Improve knowledge of contraception options — LARC methods, COC contraindications, emergency contraception; evidence via CBD and learning log" |
Every time you identify a clinical knowledge gap — whether from a patient encounter, a learning log, or AKT practice — treat it as a three-step process: (1) Identify the specific guideline; (2) Read that section of NICE CKS or BNF; (3) Write a specific PDP entry if the gap is large enough. Use RCGP GP SelfTest to do this systematically across the whole curriculum.
🗂️ Linking PDPs to the 13 Core Capabilities
PDPs should map across all five RCGP capability areas. A common ARCP pitfall is that all entries cluster around Area B — aim for breadth across the training year.
| Area | Theme | Specific Capabilities |
|---|---|---|
| A | Knowing yourself & relating to others | Communicating and consulting; Ethical approach; Fitness to practise |
| B | Applying clinical knowledge | Data gathering; Clinical examination/CEPS; Decision-making/diagnosis; Clinical management |
| C | Managing complex & long-term care | Medical complexity; Team-working |
| D | Working in organisations | Performance, learning and teaching; Organisation, management, leadership |
| E | Caring for the whole person | Holistic practice, health promotion and safeguarding; Community health and environmental sustainability |
ARCP panels consistently flag portfolios where every PDP entry addresses only clinical knowledge (Area B). Ensure at least one PDP per review period falls outside Area B. Communication and consulting, ethical practice, leadership, and community health orientation all require deliberate, evidenced development.
🧪 Learning Needs Identification Tools
RCGP GP SelfTest
Free for registrar members. 2,950+ AKT-style questions. Curriculum-wide learning needs assessment with peer comparison. Use at the start of each placement to generate specific PDP ideas from your weakest curriculum areas.
Placement Planning Meeting
Complete the specialty self-assessment handbook tool before meeting your Clinical Supervisor. Identify gaps before writing PDPs for that rotation — prevents retrospective PDPs entirely.
COTs, CbDs, Mini-CEX, MSF
Review feedback from each assessment — recurring themes across multiple assessments are strong candidates for PDP goals. If rated "Needs Further Development" on a capability, it must feature in subsequent PDPs.
PUNs and DENs
Patient Unmet Needs and Doctor's Educational Needs — the most authentic sources for PDP goals, grounded in real patient care rather than curriculum coverage.
📅 RCGP Curriculum Update — August 2025
Assessment, exams (AKT, SCA), and ePortfolio requirements are unchanged. New PDP priority themes from August 2025:
- Virtual and remote consulting competence — telephone, video, and asynchronous consultation safety
- Planetary health considerations — prescribing choices including inhaler selection
- Health equity and accessibility — recognising and addressing barriers to care
- Co-produced care plans — involving patients meaningfully in long-term condition management
Capability name updates: "Communication and consultation" → "Communicating and consulting"; "Community orientation" → "Community health and environmental sustainability".
🎯 SCA High-Yield Tips — PDP Edition
What examiners actually look for — and how a well-written PDP predicts SCA success.
There is a stronger link between the PDP and SCA performance than most trainees realise. Examiners assess whether you are the kind of doctor who identifies their own weaknesses, reflects on them, and changes their behaviour as a result. That is precisely what a good PDP demonstrates.
INSIGHT → ACTION → REASSESSMENT
The SCA specifically tests Capability A (Communicating and consulting), and examiners look for candidates who can discuss uncertainty, acknowledge limitations, and safety-net specifically — all skills linked to reflective practice nurtured by genuine PDP engagement.
⚠️ Common SCA Failures Linked to Poor PDP Thinking
| SCA Weakness | Underlying PDP Gap | What a Good PDP Would Have Done |
|---|---|---|
| Poor or generic empathy | No communication learning goals; empathy treated as innate | Specific goal to practise interpretive empathy in observed consultations with COT feedback |
| Over-referring | No decision-making reflection; no primary care confidence goal | Goal to review referral thresholds; discuss cases with trainer |
| Time mismanagement | No consultation structure goals | Goal to practise 10-minute structure with video review and trainer feedback |
| ICE missed or rushed | No patient-centred learning goals | Goal to elicit ICE within first 2 minutes for one month, with reflective log entries |
| Shared decision-making absent | No goal around eliciting patient preference | Goal to consistently offer two or more options, documented via CBD |
| Uncertainty acknowledged poorly | No PDP goal around honest communication of diagnostic uncertainty | Goal to practise specific uncertainty phrases with named triggers in consultations |
🧠 The Three SCA Domains — PDP Goals for Each
Domain 1 — Data Gathering
Collecting information efficiently, including ICE, red flags, and relevant history.
Example PDP: "Practise structured ICE elicitation within the first two minutes of the consultation and reflect on five consultations per week."
Domain 2 — Clinical Management
Sound, safe, NICE-aligned decisions — including when to manage in primary care vs refer.
Example PDP: "Develop confidence in balancing shared decision-making against doctor-led decision when clinical risk is high — evidence via CBD."
Domain 3 — Relating to Others
Communication, empathy, rapport, managing difficult moments — the domain where most marks are lost.
Example PDP: "Replace generic empathic phrases with interpretive empathy statements — practise naming what the patient is feeling, not just acknowledging it. Evidence via COT."
🌍 IMG-Specific SCA Notes — Linked to PDP Priority Areas
Medical training in many countries outside the UK is direct and medically focused — emotional acknowledgement, open-ended questions, and patient-led agenda-setting were not routine. The SCA is explicitly designed around the UK primary care consultation model, which places significant weight on the patient's perspective and active involvement in decisions. With deliberate, evidenced practice, these skills can be developed.
Highest-Yield PDP for IMGs
Targeted PDP entries around Capability 1 (Communicating and consulting) — with COTs and CbDs as evidence — are the single highest-yield investment for SCA preparation. Prioritise these from the start of training, not the month before the exam.
Mixed Peer Study Groups
A mixed peer study group — IMGs alongside UK graduates — provides insight into different consultation styles and normalises the patient-centred approach. More useful than formal teaching alone for developing natural-sounding consultation language.
Soft Skills Are Learnable
Active listening, validation, reflecting back the patient's emotional experience — these are skills, not personality traits. Write a specific PDP goal, practise in observed consultations, evidence via COT. The SCA rewards deliberate practice.
What to Include in the PDP Entry
Name the specific communication behaviour to develop. Plan specific practice with a named phrase. Evidence via COT with trainer feedback. Write a review reflection noting what changed in practice.
🩺 Case Scenario — From SCA Failure to Strong PDP
❌ Weak PDP
Goal: "Improve my empathy in consultations."
Action: "Be more empathetic."
Evidence: (blank)
No insight, no plan, no measurable change. The ARCP panel cannot assess whether anything improved.
✅ Strong PDP
Goal: "Develop interpretive empathy — naming and reflecting the patient's emotional experience rather than using generic phrases."
Action: "Practise reflective statements in 5+ consultations per week. Two COTs with trainer. Read Calgary-Cambridge communication model."
Evidence: "Two COTs with feedback; five annotated log entries."
By: End October 2026.
Examiners are not impressed by empathy — they are impressed by specific empathy. "That sounds hard" is a phrase. "It sounds like you felt completely alone with this, and that nobody was taking you seriously" is interpretive empathy. The second version costs no extra time and scores significantly higher marks. Build it as a PDP goal before your SCA, not after.
- PDP goals that describe what you want to feel but not what you will do — "be more confident" is not a goal
- Communication goals with no planned evidence — empathy cannot be assessed without observation
- SCA preparation that is all clinical knowledge revision with no consultation skills work in the PDP
- A PDP with zero goals related to Domain 3 (Relating to Others)
- A PDP with zero goals outside Capability Area B — ARCP panels flag this explicitly
🎭 SCA-Linked Worked Case Examples
These cases show exactly what separates a weak SCA candidate from a high-scoring one — and how clinical knowledge translates into consultation performance.
🩹 Case 1 — Acute Low Back Pain (No Red Flags)
❌ Weak Candidate
- Orders MRI lumbar spine "to be safe"
- Provides no explanation of what is causing the pain
- Offers no reassurance about prognosis
- Gives no timeline
- No safety-netting for red flags
✅ High-Scoring Candidate
- Actively excludes red flags (bladder/bowel, bilateral neurology, saddle anaesthesia)
- Explains mechanical nature clearly
- Gives a realistic, reassuring timeline
- Recommends staying active, analgesia, and self-care
- Explicit safety-netting for cauda equina symptoms
- "The good news is this doesn't sound like anything serious — most back pain like this is mechanical, which means it's related to the muscles and joints rather than anything worrying."
- "I'd actually recommend staying as active as you comfortably can — rest tends to make it take longer to settle."
- "Most people find it improves significantly within 4 to 6 weeks. If it hasn't improved by then, come back and we'll reassess."
- "If you notice any change in bladder or bowel function, or weakness in both legs — that's something I'd want you to go to A&E about straightaway."
The clinical knowledge is: no red flags = no imaging; conservative management is first-line. The SCA tests: can you communicate that decision convincingly, with reassurance, a timeline, and specific safety-netting?
🤧 Case 2 — Viral Cough (Patient Expecting Antibiotics)
❌ Weak Candidate
- Prescribes antibiotics to avoid conflict
- Provides no explanation of why antibiotics are inappropriate
- Caves immediately when the patient pushes back
- No safety-netting for features of bacterial infection
✅ High-Scoring Candidate
- Acknowledges the patient's expectation without immediately agreeing
- Explains the viral nature and why antibiotics wouldn't help
- Mentions antibiotic side effects and resistance — briefly, not lecturing
- Offers practical self-care alternatives
- Provides explicit safety-netting for secondary bacterial infection
- "I can see why you'd think antibiotics might help — a lot of people feel that way, and it's a really understandable thought."
- "Antibiotics wouldn't help here and can actually cause some unpleasant side effects — and using them when we don't need to makes them less effective for the future."
- "If you develop breathlessness, chest pain, or if the cough hasn't improved in 3 weeks, please come back and see us — those would be reasons to look more carefully."
🩸 Case 3 — Mildly Raised PSA (Worried Patient)
❌ Weak Candidate
- Immediately refers under 2WW "to be safe"
- Does not explain that PSA needs repeating
- Does not mention confounders (UTI, vigorous exercise)
- Escalates patient's anxiety unnecessarily
✅ High-Scoring Candidate
- Acknowledges the patient's worry specifically and interpretively
- Explains that a mildly raised PSA needs repeating before any further action
- Explains confounders that can temporarily raise PSA
- Plans repeat PSA with a clear follow-up and safety-netting
- "I can completely understand why a result like this would worry you — and I want to make sure we handle this properly."
- "PSA is a useful test, but it can be raised by things other than prostate cancer — like a urine infection, or vigorous exercise before the test. So before we do anything, the right thing is to repeat it."
- "If the repeat comes back normal, we can be more reassured. If it's still raised, we'll talk about what the next step should be."
🔁 GP Practical Framework
How to embed the PDP into your real working day — not just your ESR preparation.
The most effective PDP entries begin in clinic — with a moment where something did not go quite right. The skill is learning to catch those moments and convert them into structured learning goals before they fade.
- Identify your learning need — from multiple sources
Complete RCGP GP SelfTest or specialty self-assessment tool before each placement planning meeting. Review feedback from COTs, CbDs, MSF. Check your last ESR: which capabilities are rated "needs further development"? Those must feature in subsequent PDPs.
- Write the PDP entry — SMART from the start
Name the specific learning need (not a broad domain). Write an action plan with named activities — which specific NICE CKS section, which clinic to attend, which module to complete. Set a realistic target date and state exactly how you will know the goal is achieved.
- Take action and document it
Attend the clinic, complete the module, attend the course. Write a CCR at the time. Upload any certificate to FourteenFish as a CPD entry. Link the CCR to the PDP entry via "Send to PDP". Do this at the time — not weeks later.
- Apply the learning in practice
See a patient where the newly acquired knowledge is relevant. Write a follow-up CCR explicitly linking to the previous learning: "Following my learning about COPD management last month, today I managed a patient with an exacerbation in the following way…" This closes the learning loop.
- Review and reflect on the PDP entry
In the review field on FourteenFish, complete the reflection: "Did I achieve this goal? What challenges did I face? Has this generated a new learning need?" Mark the entry as completed, carried forward, or modified with a reason.
- Present at your ESR
Review all current PDPs — flag which have been achieved, which to carry forward, and propose new entries. Ensure at least two PDP entries are active per training year with progress demonstrated in at least one. Arrive with draft goals and use the ESR to refine them with your supervisor.
- Safety-net your own learning
If a rotation ends before you complete a PDP, carry it forward explicitly — unexplained incomplete PDPs are flagged. Use study leave proactively to address persistent gaps; study leave must be congruent with GP curriculum learning outcomes. If a more important need emerges mid-post, update the plan and document why.
🏆 The Gold Standard PDP Loop
The Gold Standard PDP Loop
Learning loop CLOSED ✓ — This is what a commendable ePortfolio looks like to an ARCP panel.
📋 Worked Example — Complete PDP Entry (Loop Closed)
| Trigger (Case) | Patient with unexplained weight loss and change in bowel habit. Unsure whether the combination met 2WW criteria and hesitated before referring. Patient had to return the next day after I had checked the guidelines. |
| Gap (DEN) | Knowledge gap — specific 2WW criteria for colorectal cancer, FIT threshold, and age-symptom combinations. Logged as DEN in CCR entry. |
| PDP Goal (SMART) | Review NICE NG12 2WW colorectal criteria — age thresholds, symptom combinations, when FIT ≥10 applies. Complete by end September 2026. |
| Actions Taken | Read NICE CKS colorectal cancer recognition page; created one-page summary card; discussed with trainer at tutorial; RCGP e-learning certificate uploaded to FourteenFish as CPD entry. |
| Loop Closed | "Following my learning about 2WW colorectal criteria, today I managed a patient aged 52 with rectal bleeding and looser stools. Applied FIT test appropriately and referred under 2WW with confidence. CBD completed with trainer confirming appropriate clinical reasoning." — CCR dated [date]. |
| Review | Goal achieved. No longer hesitating. New learning need: PSA thresholds by age — will write further PDP for next review period. Closed October 2026. |
A consistently poor or absent PDP does not just risk your ARCP outcome. Under GMC revalidation requirements, all licensed GPs must demonstrate CPD and reflective practice. A GP who cannot identify their own learning gaps is a patient safety risk. Good PDP habits are a professional safeguard, not just a training requirement.
⚠️ Common PDP Pitfalls
The mistakes trainees make most often — and how to avoid them.
- Writing it the night before the ESR. The PDP is supposed to be a living document. Creating all your PDPs in the week before your ESR signals that the process is not integrated into real learning.
- Setting goals that are too broad. "Improve my clinical knowledge" is not a PDP entry — it is a life plan. Narrow it down to one specific area with specific actions.
- "Pass AKT" or "Write more log entries" as PDP goals. The RCGP explicitly cites both as unacceptable. They are national requirements for all trainees, not personal learning needs.
- All PDPs in the same capability area. Trainees frequently write multiple PDPs around clinical knowledge (Area B) but neglect communication, ethics, leadership, and community orientation (Areas A, D, E). Aim for at least one entry outside Area B per review period.
- No evidence planned upfront. Always state what evidence you will provide — a certificate, a CBD, a COT. Entries where certificates are uploaded but no subsequent CCR demonstrates application of the learning are explicitly flagged.
- Failing to close the learning loop. If you complete an e-learning module but never write a follow-up CCR showing how that changed your practice, the loop is open. Open loops are noted by supervisors and ARCP panels.
- Leaving the "How will I know when it's achieved?" field empty. Keep it simple: "I will be able to manage this independently, evidenced via CBD."
- Not updating the PDP during the post. PDPs not updated since the last ESR suggest passive engagement and are flagged at ARCP. Update it as you go — even briefly.
- Using the PDP to tick boxes, not to direct learning. Trainees who write PDPs reactively — after identifying what has already been done — miss the true value: prospective planning that shapes clinic attendances, courses, and supervisory sessions.
- Hospital-rotation PDPs that are not GP-relevant. Always ask: "How does this help me as a future GP?" Learning LSCS technique is not GP-relevant. Counselling patients about elective LSCS, risks, and recovery is.
- Copy-pasting PDP entries between review periods. Identical or near-identical entries suggest the PDP is not being treated as a living document. Supervisors and ARCP panels notice this consistently.
- Writing PDP goals that describe feelings, not actions. "I want to feel more confident with dermatology" is a wish. "I will complete the Primary Care Dermatology Society online module and review 10 lesions with the practice's skin lead by October 2026" is a goal.
- Ignoring it post-CCT. The training PDP transitions directly into the appraisal PDP. Appraisal is mandatory for revalidation. A poor training PDP is a poor start to your professional career.
🛠️ Practical Shortcuts That Actually Work
"Send to PDP" Button — Use It Every Time
At the end of a CCR, clicking "Send to PDP" transfers the identified learning need directly into the PDP section. Do this the moment a DEN is identified — not weeks later from memory.
Start the PDP at the Placement Planning Meeting
Use the specialty self-assessment handbook tool before meeting your Clinical Supervisor. Identify gaps and write your first PDPs for that rotation at the meeting — before seeing a single patient. Prevents retrospective PDPs entirely.
Plan Study Leave Around PDP Goals
If you have a PDP on managing acute eye conditions, book study leave at an ophthalmology clinic. Study leave must be congruent with GP curriculum learning outcomes — making it PDP-linked is efficient and prevents unjustifiable study leave requests.
Use RCGP GP SelfTest to Generate PDP Ideas
Complete a curriculum-wide learning assessment on GP SelfTest, identify your weakest topic area, and write a SMART PDP around it. The most systematic way to ensure PDPs cover the full curriculum.
Link PDPs to Your ESR Capability Ratings
If rated "Needs Further Development" on a capability at an ESR, that capability must feature in at least one subsequent PDP entry. Supervisors check for this explicitly.
Set Two Calendar Reminders Per Review Period
At 6 weeks and 10 weeks — labelled "PDP check-in." These 10-minute sessions prevent the ESR-eve panic that produces weak, last-minute entries.
Patterns that risk Outcome 2 (additional requirements without extra time):
- No active PDPs in the ePortfolio
- All PDPs incomplete — created but never reviewed or reflected on
- No breadth — all entries address only one capability area
- PDPs not updated since the last ESR
- No evidence of application — certificates uploaded but no CCR showing learning applied in practice
Contribution to Outcome 3 (additional training time required):
- A consistently poorly maintained PDP is documented within the ES report, contributing to unsatisfactory WPBA judgment which can trigger Outcome 3 alongside other concerns
Experienced Educational Supervisors can spot a PDP written in 20 minutes the night before an ESR: goals that have no connection to any learning log entries, and goals marked as "achieved" with no evidence attached. The trainees whose PDPs stand out write entries that feel personal, specific, and connected to real clinical experiences.
🧠 PDP Cheat Sheet
The one-page summary you'll want before every ESR.
| Question | Answer |
|---|---|
| What is a PDP? | A structured plan for bigger, chunkier learning needs — not a learning log and not a to-do list |
| RCGP minimum per training year? | 2, with progress demonstrated in at least one; good practice is 3+ per clinical placement |
| Where do ideas come from? | Learning logs, patient encounters, PUNs/DENs, COT/CBD feedback, GP SelfTest, placement planning meeting, ESR capability ratings |
| What framework? | SMARTIES / SMAARTER+ — Specific, Measurable, Achievable, Aligned, Relevant, Time-bound, Evaluated, Reviewed, + Impact documented |
| Types of learning? | Knowledge (K), Skills (S), Attitudes (A) — state which one your goal addresses |
| What evidence? | Plan upfront: course certificates, CCR reflections, CBDs, COTs, Mini-CEX — and a follow-up CCR showing application in practice |
| NOT acceptable? | "Pass AKT", "Write more log entries", or any minimum training expectation — explicitly unacceptable per RCGP |
| Capability Area trap? | Do not cluster all entries around Area B (clinical knowledge) — ensure breadth across Areas A, C, D, E too |
| FourteenFish process? | Review progress → Suggest new entries → Agree with ES — in that order; skipping stages breaks the system |
| Post-CCT? | Your training PDP becomes the foundation of your post-CCT appraisal PDP and lifelong revalidation cycle |
IDENTIFY → PLAN → ACT → EVIDENCE → APPLY → REFLECT → UPDATE → REPEAT
The loop is only complete when the learning has been applied in practice and the impact documented. Stopping at "EVIDENCE" is the most common portfolio weakness at ARCP.
💎 Insider Pearls
Real-world wisdom from GP trainees and trainers — the things nobody tells you at the start.
Link everything to a log
The most convincing PDPs are clearly rooted in a specific learning log entry. When your ES or ARCP panel sees "this need arose from learning log entry X," it shows self-awareness and genuine reflection — not just paperwork.
What ARCP panels love to see
A PDP updated mid-post — not just at ESR time. Changes documented with a reason. Entries closed with evidence. Goals that feel personally meaningful, not bureaucratically selected.
The diary reminder trick
Set two calendar reminders at the start of each review period: 6 weeks and 10 weeks — labelled "PDP check-in." These 10-minute sessions prevent the ESR-eve panic that produces weak, last-minute entries.
Carry-forward is fine
Not every PDP goal needs to be completed within one review period. Larger goals may carry forward across two ESR periods. What matters is active engagement — evidence of progress, even if incomplete.
Quick and rough beats nothing
A rough note is better than a blank page. You can always refine it later. A brief, honest entry with plans to develop it is far better than a complete entry written entirely in retrospect.
For IMGs especially
PDP is often unfamiliar for doctors trained outside the UK. The key mindset shift: this is not about self-criticism — it is about demonstrating that you are an active, self-directed learner. Avoid copying entries between review periods — supervisors notice this consistently.
The capability coverage shortcut
Check your FourteenFish curriculum coverage dashboard at the start of each review period. Areas with thin evidence are instant PDP candidates — write a targeted goal and simultaneously plan log entries and WPBAs that will strengthen that capability.
Your ESR is a conversation, not a performance
Arrive with draft goals and use the meeting to refine them with your ES. The best PDPs are co-constructed — not submitted in advance as a fait accompli. Your supervisor often has excellent insight into which needs are most pressing for your stage.
💡 What I Wish I Knew
The ARCP panel, your ES, and — eventually — your appraiser are all looking for the same thing: a doctor who knows what they do not know, has a plan to address it, and can demonstrate they followed through. Treat it as a professional record of your growth, not a portfolio obligation.
Three things. Specificity — a goal precise enough that you could explain it to a patient. Relevance — clearly linked to your clinical practice. Evidence of change — some demonstration that the learning made a difference. It does not need to be elaborate. It needs to be genuine.
Before submitting any PDP entry, ask yourself:
"If the ARCP panel read this PDP entry — would they know what you actually learned, how you learned it, and how it changed your practice?"
If the answer is not clearly yes — revise the entry before you submit it.
🧑🏫 For Trainers: Teaching the PDP
Common trainee blind spots, tutorial ideas, and discussion prompts.
Common trainee blind spots on PDPs
- Confusing the PDP with the learning log. Many trainees write PDP entries that are more like log reflections — describing what happened rather than planning what they'll do next. Redirect: "What is your plan to address this need?"
- Choosing comfortable goals. Trainees often gravitate towards areas they already find interesting. Gently challenge them to identify a genuinely difficult area — one that makes them slightly uncomfortable. That's where growth happens.
- Passive goals. "Read about X" or "attend tutorials" without specifics. Encourage concrete plans: which course, which guidelines, which supervisor to sit in with, by what date.
- No evidence mapped out. Introduce the habit early: "What will you show me to prove you've done this?"
- All PDPs in the same capability area. Ask trainees to audit their PDP entries across the five areas A–E. If everything is in Area B, redirect towards Areas A, D, or E for the next entry.
- Treating the PDP as a confidential document. Create a psychologically safe space where identifying gaps is celebrated, not penalised.
Tutorial Ideas and Discussion Prompts
🔍 Scenario: The reluctant PDP trainee
Your ST2 arrives at their ESR. Their PDP has two entries, both written that morning, both vague. Explore why the PDP felt like a burden and co-create what a genuinely useful PDP would look like for their remaining post.
Discussion prompt: "If you could learn one thing in GP that would make you a noticeably better doctor in six months, what would it be?"
📝 Exercise: From log to PDP
Take a recent learning log entry together and work through it: Does this identify a PDP-worthy learning need? How would we write a SMART goal from this? What actions would it involve? How would we know when it's achieved?
This demystifies the process and shows trainees that PDP writing doesn't have to start from a blank page.
⚖️ Teach the difference: PDP vs learning log
Give trainees two examples side by side — one that belongs in a learning log, one that warrants a PDP entry. The key differentiator: if it can be done in an evening, it's a log entry. If it needs a plan, a timeline, and multiple activities, it's a PDP.
🎯 Reflective questions for advanced trainees
"Your training finishes in three months. If your PDP becomes your first appraisal PDP next year, what would you want it to say about who you are as a learner and a doctor?"
Also: "If the ARCP panel read your PDP today — would they know what you actually learned, how you learned it, and how it changed your practice?"
The most powerful thing you can do as a trainer is model good PDP thinking. Share your own appraisal PDP with your trainee (with appropriate discretion). When trainees see that experienced GPs continue to identify learning needs and plan development goals, the PDP stops feeling like a training exercise and starts feeling like a professional habit.
❓ Frequently Asked Questions
The questions trainees ask most — answered directly.
How many PDP entries should I have per review period?
The RCGP minimum is 2 per training year with progress demonstrated in at least one. Good practice is 3 per clinical placement. Three well-written, completed entries beat eight vague, unfinished ones every time.
Is there a pass mark for PDPs?
No formal pass mark — but ARCP panels assess whether your PDP demonstrates genuine engagement with self-directed learning. A consistently poor PDP can contribute to an ARCP Outcome 2 or Outcome 3. Treat it seriously.
Can I change my PDP during the post?
Yes — you're encouraged to. PDPs should be dynamic documents. If a more important learning need emerges, update the plan and document why. Just don't use "I changed my mind" as a way to delete goals you didn't get around to completing — document the reason honestly.
What if my ES disagrees with my PDP goals?
This is a healthy conversation. Your ES's role is to help you prioritise — they may redirect you towards areas they've noticed are more pressing. The agreed PDP is collaborative. If you feel strongly about a goal your ES has deprioritised, have that conversation openly — and document it.
I'm an IMG — where do I start?
Start by understanding that the PDP is not about self-criticism — it's about demonstrating that you actively identify your own learning gaps and take responsibility for addressing them. Begin with one area where you genuinely feel less confident in UK primary care context. Prioritise Capability A (communicating and consulting) PDPs from the outset — this is the domain most often tested in the SCA.
Can I use my PDP to address exam preparation?
Only if it's specific. "Pass the AKT" is explicitly unacceptable. But "I've noticed from practice questions that I repeatedly struggle with cardiac arrhythmias — I plan to work through the relevant NICE guidelines, complete an online module, and discuss three cases with my trainer by December 2026" — that is a specific, SMART PDP.
What happens to my PDP after I qualify?
It continues. Every GP must maintain an active PDP as part of their annual appraisal, which is mandatory for revalidation. The habits you build during training — identifying learning needs, planning development goals, providing evidence — continue throughout your career.
The "How will I know when it's achieved?" box always trips me up.
Approaches that work:
- "I will be able to manage this presentation confidently and independently in clinic."
- "I will have completed [specific course/CBD/COT] and written a reflection demonstrating what I've learned."
- "My ES will confirm through CBD/COT that I have demonstrated improvement in this area."
- "I will no longer feel the need to look this up during or after the consultation."
Keep it honest and simple. The goal is a shared understanding of what "done" looks like.
🏁 Final Take-Home Points
- 1.The PDP is for bigger, chunkier learning needs — things that need planning, time, and multiple activities. Everyday learning belongs in the learning log.
- 2.RCGP minimum: 2 per training year, with progress in at least one. Good practice: 3 per clinical placement. Quality beats quantity every time.
- 3.Every learning need is Knowledge, Skills, or Attitudes. State which one. It makes goals sharper and gives your supervisor and ARCP panel clarity.
- 4.Close the learning loop. Plan your evidence upfront, apply the learning in practice, write a follow-up CCR, and document the impact. Stopping at "uploaded certificate" is the most common portfolio weakness at ARCP.
- 5.Aim for breadth across all five RCGP capability areas. At least one PDP per review period should fall outside Area B (clinical knowledge).
- 6.Update your PDP during the post — not just at ESR time. Set two calendar reminders per review period. Ten minutes every six weeks beats two hours the night before your ESR.
- 7.A poor PDP can contribute to ARCP Outcome 2 or Outcome 3. A good PDP demonstrates that you are a self-aware, proactive, safe learner. The bar is real — but it is not impossibly high.
- 8.From August 2025, ensure PDPs increasingly reflect the updated RCGP curriculum: virtual consulting, planetary health, health equity, co-produced care.
- 9.Ground every PDP entry in a real clinical experience. If you can reference a specific learning log (CCR), even better — it shows the PDP is driven by genuine practice, not bureaucracy.
- 10.Your training PDP becomes your appraisal PDP. The habits you build now — identifying gaps, planning development, providing evidence, reflecting on change — are lifelong professional skills and a foundation of safe practice.
Created with care by Dr Ramesh Mehay and the Bradford VTS team.
Page content is for educational guidance. Always refer to your deanery, the RCGP, and FourteenFish support for current requirements.
A database of PDP actions
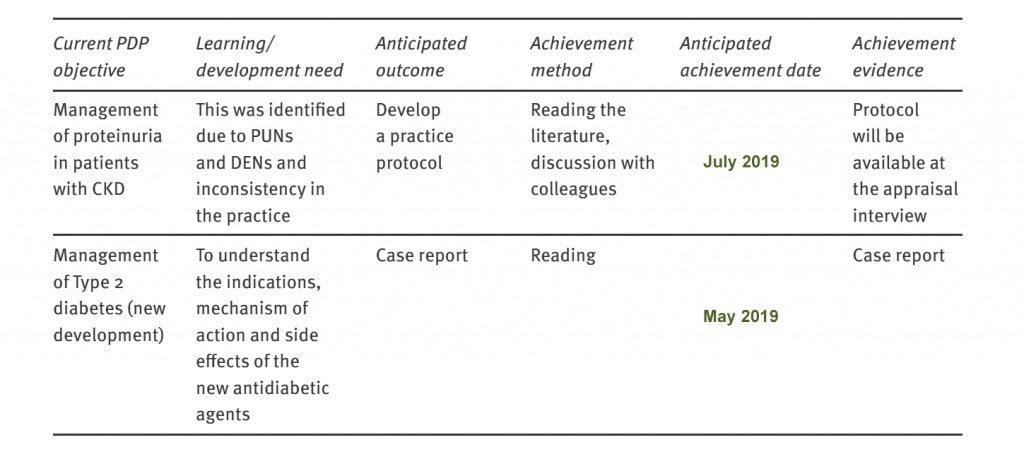
WHAT
To keep up to date with new clinical developments
HOW
Attend tutorials
WHEN
Over next 6-12 months
OUTCOME
Pass exams and assessment
Learn about gynaecology as applied to general practice
Attend tutorials and ward rounds during ST2 job in O&G
Over next 6 months
Be more confident
Become more proficient, thorough and confident in taking sexual health histories
Practice within joint consultations
During GU attachments during O&G job
Improve proficiency as shown through a relevant CBD and mini-CEX
Which of these are good and which are bad?
Answers:
The first one is not SMART, as the objective is broad and general. There is no measurable or specific endpoint – when does a doctor finish keeping up to date? The second one is not SMART for the same reasons as above. The third one is good – the need for this objective was identified during a clinical encounter and recorded in the shared log. So the answer is – The 3rd is good, but 1 and 2 are bad.
- Specific: they should relate to specific tasks/activities, not general statements.
-
- BAD: “I want to improve my consultation skills”
- BETTER: “I want to learn some Motivational Interviewing techniques” or “I want to learn techniques to diffuse the angry situation”
-
- Measurable: it should be possible to assess whether they have achieved.
-
- BAD: “I will show improvement through my daily consultations”
- BETTER “I will have attended a course and will write up some reflections. I will also document 3 consultations where I have used these new techniques”
-
- Achievable: it should be possible for the doctor to achieve the desired outcome.
-
- BAD: “I want to learn everything about Women’s Health because it is a weak area of mine”
- BETTER “I want to improve my knowledge in common Women’s Health areas – namely menstruation difficulties, contraception and the menopause”
-
- Relevant: objectives should be appropriate for the current role and situation.
-
- BAD: “I want to improve my knowledge of rare neurological disorders” (Why if you’re not going to be a neurologist?”
- BETTER: “I want to improve my knowledge of MS and the services available” (Because MS is not uncommon in General Practice)
-
- Time-bound: there should be a clear time frame set in which to achieve objectives.
-
- BAD: “I will do this soon”
- BETTER: “I will do this before September 2020” or “I have found a Motivational Interviewing course schedule for Sept 2020 in Birmingham and will attend that and write up reflections aafterwards.
-
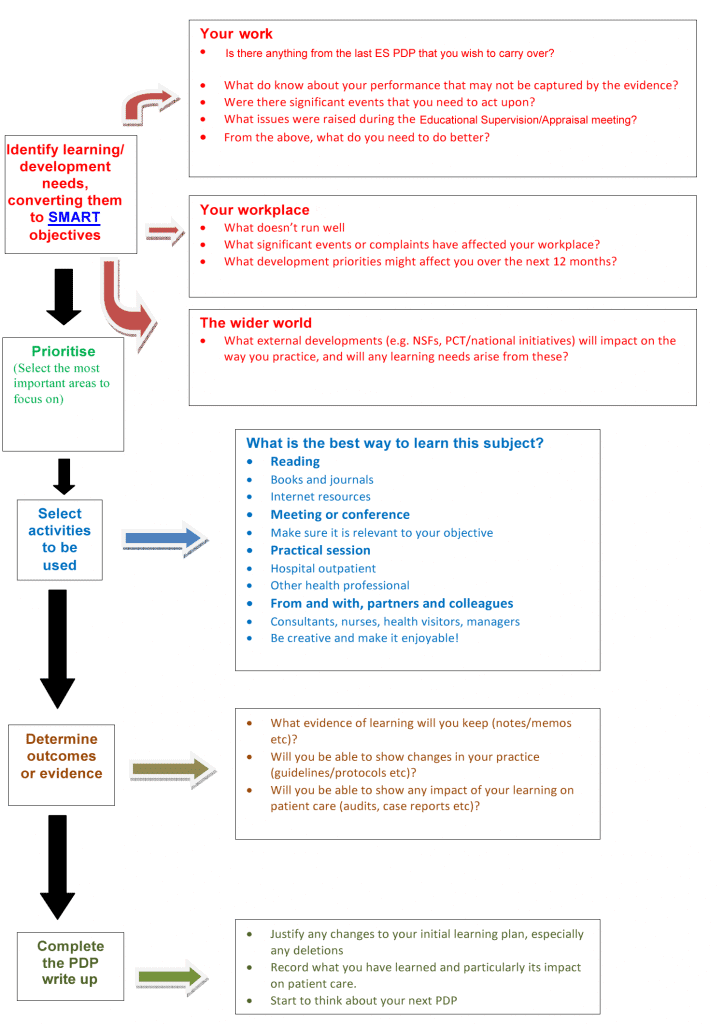
And finally
A great little infographic from Amar Rughani & Nick Field. I think this summarises everything nicely.

Thank you for this comprehensive information on PDPs.